COVID-19 has left no community untouched. But its disproportionate impact on our most vulnerable populations — particularly communities of color — is well documented. Sadly, this holds true across the nation and in California, where the death rate is 22% higher for Latino people and 8% higher for Black people than the overall statewide death rate, and the COVID case rate is 32% higher for Pacific Islanders. COVID case rates for poorer communities — those with a median household income below $40,000 — have been 37% above statewide rates as well.
For these communities, health disparities and mistreatment aren’t new. Historical and systemic racism has, and continues to, exclude people of color from accessing health care and social services. The cultural identities and the language of communities of color have been threatened for decades. That experience has been compounded by community leaders and elders being disproportionately affected by COVID, making the need to proactively protect their cultural identity and heritage even greater. And California’s immigrant communities, which have faced these inequities throughout their history, have been forced to choose between their jobs and their health during the pandemic. As vaccination efforts continue, these communities still face a lack of equity in distribution, though availability is on the rise across the population.
Understanding Hesitancy
From the Tuskegee Syphilis Experiments and the use of Henrietta Lacks’ cancer cells without consent or compensation to the forced sterilization of women of color, a history scarred by systemic racism, exclusion and trauma has led to an understandable distrust of health care delivery systems within communities of color.
But through education and more awareness of the vaccine, hesitancy rates in the U.S. are dropping, and the latest U.S. Census data shows people of color aren’t more hesitant to get the vaccine than the rest of the population. Researchers found that approximately 12% of Black and white adults were equally concerned about getting it, compared with 10% of Hispanic adults who felt similarly.
Despite this good news, we’ve observed that vaccine distribution has not been equitable, and community and health care leaders across the country have been working together to pop up vaccine clinics in communities of color, offer more walk-in appointments to improve access and find other strategies to ensure a more equitable distribution.
An Opportunity to Promote Equity
As dire as the circumstances of this pandemic have been, we are strengthened by the knowledge that we have an opportunity to ensure health equity for all Americans. Many leaders across multiple sectors have joined in this fight, providing proactive outreach in communities that have been disproportionately affected, historically disenfranchised or have more limited access to health care.
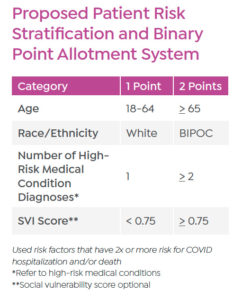
At CommonSpirit Health, we’ve been leading the effort to develop a vaccine outreach prioritization matrix. While some outreach is afforded to all patients, this tool focuses additional and more intensive outreach to populations at higher risk (as defined by the CDC) from COVID-19 infection.
We asked leaders in our markets throughout the U.S. to consider adopting this evidence-informed tool to guide their outreach planning and programming. All patients should receive some communication, with at-risk individuals scoring higher on this scale receiving intentional outreach. This outreach should include culturally competent education/awareness, helping patients make a plan to get their vaccine (and navigate the sometimes-confusing registration processes), and support in addressing potential barriers and/or hesitancy to vaccination.
One of my favorite quotes from Martin Luther King Jr. is: “Of all the forms of inequality, injustice in health care is the most shocking and inhumane.” If we want to move past this pandemic and work toward a stronger, more equitable health care delivery system, we must ensure that everyone has the same opportunity to access this lifesaving vaccine.